Autonomic nervous system
The autonomic nervous system or ANS for short, is the part of your nervous system that takes care of your heart rate, breathing, digestion, blood pressure and so on, basically all the processes in your body that you don't have to think about doing. We've included an explanation of a particular part of the nervous system here because understanding your ANS is like getting the user manual for your emotional life, it helps you decode why you react the way you do, especially under stress, or following a traumatic event or difficult childhood experiences. If you feel overwhelmed by your feelings or hijacked by uncomfortable body sensations, we have some helpful tools in Create My Toolbox
The facts....
We will start by saying that the following explanation is a very simplified version of a very complex system, hopefully there's enough information here to give you an overview that will give you some understanding:
The nervous system has two main parts:
The Central Nervous System (CNS): made up of your brain and spinal cord, the brain reads signals from your nerves to regulate how you think, move and feel.
Peripheral Nervous System (PNS): made up of a network of nerves which branch out from your spinal cord. This system relays information from your brain and spinal cord to your organs, arms, legs, fingers and toes.
There are two parts to your peripheral nervous system:
The Somatic Nervous System (SNS)
This system handles voluntary control—everything you consciously do.
Sensory neurons: Carry information from sensory organs (skin, eyes, ears) to the central nervous system (CNS)
Motor neurons: Transmit signals from the CNS to skeletal muscles to produce movement
Reflex arcs: Enable fast, automatic responses without involving the brain (e.g., pulling your hand away from a hot surface)
🦵 Example: Walking, talking, typing, or reacting to pain
Autonomic Nervous System (ANS)
This system manages involuntary functions—processes you don't consciously control. For example, heart rate, digestion, respiration, pupil dilation, and glandular activity.
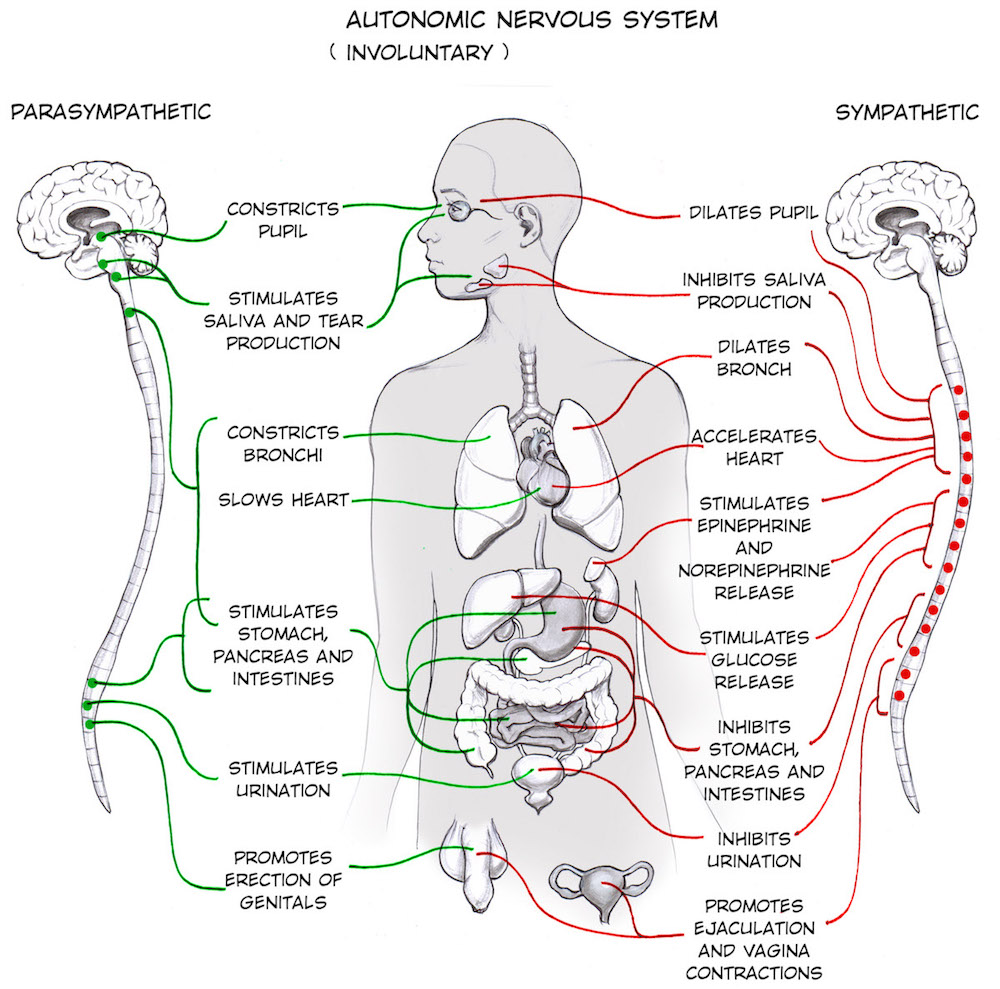
It is subdivided into the:
Sympathetic Nervous System: Prepares the body for action, its our fight or flight response to perceived threat or danger, a survival instinctual response that kicks in to protect us
Parasympathetic Nervous System: Relaxes and calms the body down after a period of stress or danger, its also called 'rest, digest and connect', which can only happen when our sense of safety is restored.
Enteric Nervous System: Independently governs digestion in the gut
🫀 Example: Your heart speeding up when you're stressed, or your stomach digesting food without you thinking about it.
The two systems often work in opposition to maintain the body's internal balance or homeostasis, its always active, even when your are asleep.
What is the Vagus Nerve?
The vagus nerve is a key component of the PNS, it is the tenth cranial nerve, and one of the longest nerves in the body, extending from the brainstem down to the abdomen. It plays a vital role in the autonomic nervous system. Dr Stephen Porges developed a theory called polyvagal theory that explains its role in emotional regulation and social behaviour which is now used in psychotherapy.
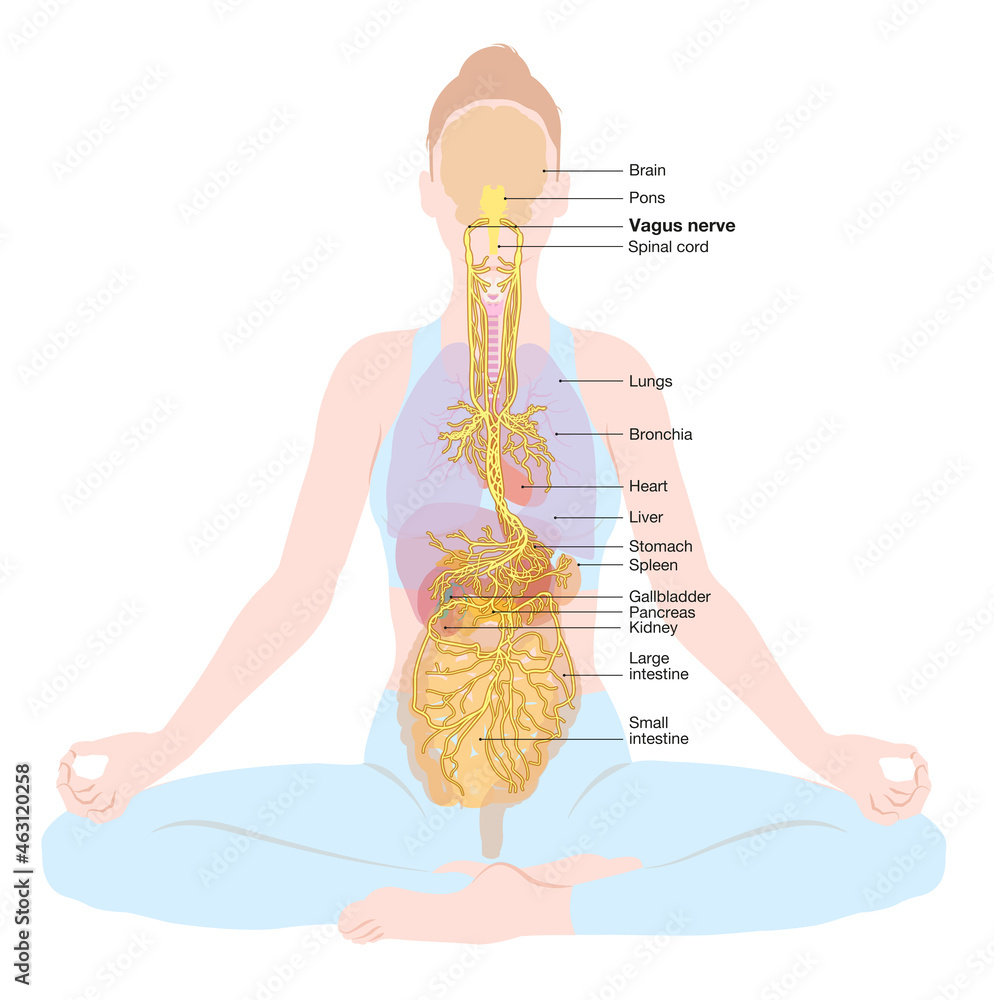
The theory identifies a hierarchy of three physiological states:
- Safe & Social (Ventral Vagal State): This is the "all clear" mode. When we feel safe and connected, the ventral branch of the vagus nerve dominates. In this state, our heart rate is calm, we can interact socially, and we feel grounded and socially engaged (for example, comfortable making eye contact and communicating). You can think of this as the body's green light – it's okay to relax, play, and connect with others.
- Fight or Flight (Sympathetic State): This is the "danger – take action!" mode. If our unconscious nervous system senses a threat, it shifts into the sympathetic nervous system drive. Adrenaline kicks in, heart rate and breathing speed up, and we become anxious, agitated, ready to fight or run away. You might notice this state when you feel angry, frightened, or intensely stressed – your body is mobilizing to protect you. (It's like the body's yellow light – proceed with caution and prepare to act.)
- Freeze or Shutdown (Dorsal Vagal State): This is the "extreme danger – shut down" mode. If a situation feels inescapably threatening, the dorsal branch of the vagus nerve takes over and essentially hits the brakes hard. In this state, heart rate and blood pressure drop, and we might feel frozen, numb, dizzy, or disconnected – like a turtle retreating into its shell. It's the body's red light – a last-resort protective response (think of a possum playing dead or a person in shock becoming unresponsive).
According to polyvagal theory, our nervous system continuously (and subconsciously) monitors our environment for signs of safety or danger – a process called neuroception. Based on what's detected, the body will automatically switch into one of the above states without conscious thought. For example, a friendly face and gentle voice can cue our body to stay in the safe social state, whereas a sudden loud noise might trigger a quick jump into fight-or-flight before we even realize it.
Why It Matters
Polyvagal theory matters because it provides a biological framework for understanding our emotions and behaviours, especially in relationships and in trauma. It highlights that feeling safe is not just an emotional concept but a physiological state. When we (or others) are in a ventral vagal state, we are capable of social engagement, communication, and learning. But when we shift into fight-or-flight or freeze, our body is focused purely on survival – which can explain behaviours like anxiety, aggression, or shutting down in the face of stress.
This understanding is very useful in fields like mental health and education. For instance, therapists use polyvagal theory to help trauma survivors by first establishing a sense of safety (bringing them back to the ventral vagal state) before processing difficult memories. It also emphasizes co-regulation – the idea that we can help regulate each other's nervous systems. Have you noticed how a calm person can soothe an anxious friend, or how a parent's gentle presence calms a frightened child? That's co-regulation in action: one person's steady ventral state reassuring another's nervous system that there is no danger. Ultimately, polyvagal theory reminds us that our bodies have an inherent system for protecting us, and understanding it can help us manage stress, improve social bonds, and foster emotional resilience by working with our nervous system rather than against it.
The feels....
Here are three fictional descriptions of what its like to have a nervous system that has become overly sensitive and what helped:
"I Didn't Know My Body Was Stuck in Survival Mode"
I used to think I was just "bad at handling stress." I'd wake up already tense, my heart racing before I even got out of bed. The smallest things—an unexpected email, a crowded room, someone's tone of voice—could send me spiralling. I wasn't just anxious. I felt like I was constantly bracing for impact, even when nothing was happening.
My body was always on high alert. I couldn't sleep through the night. My digestion was a mess. I'd get dizzy, sweaty, and short of breath in situations that didn't seem threatening to anyone else. And when I wasn't in fight-or-flight mode, I'd crash into exhaustion—numb, disconnected, unable to move or care.
I didn't understand what was happening until a therapist explained that my autonomic nervous system was dysregulated. My sympathetic system—the part that prepares you to fight or flee—was stuck in overdrive. And my parasympathetic system—the part that helps you rest and recover—was barely functioning. I wasn't broken. My body was trying to protect me, but it had lost the ability to reset.
Learning about Polyvagal Theory changed everything. I realized my nervous system wasn't just reacting to the present—it was shaped by years of unresolved trauma, chronic stress, and emotional neglect. My body had learned that the world wasn't safe, and it was doing its best to keep me alive.
Recovery hasn't been linear. I've had to relearn how to feel safe. Breathwork, somatic therapy, and even humming or gentle movement have helped me reconnect with my body. I still have days where I feel hijacked by my nervous system, but now I understand what's happening—and I have tools to come back to myself.
"Living in a Body That Won't Power Down"
I used to think I was just a worrier. I'd lie awake at night, rehearsing conversations I hadn't had yet, catastrophizing outcomes that hadn't even begun to unfold. My mind was a constant hum—like a machine that couldn't switch off. But it wasn't just mental. My body felt like it was wired wrong.
Even on calm days, my chest would tighten for no reason. My heart would flutter, my stomach would churn, and I'd feel this creeping sense of dread—like something bad was about to happen, even though everything was fine. I'd get lightheaded in meetings, feel shaky in line at the grocery store, and sometimes burst into tears without knowing why.
Eventually, I was diagnosed with Generalized Anxiety Disorder, but what really changed things was learning that my autonomic nervous system was dysregulated. My sympathetic system—the part that's supposed to activate in emergencies—was stuck in overdrive. And my parasympathetic system—the part that's meant to calm me down—was barely functioning.
It was like my body had forgotten how to feel safe.
I learned about neuroception, the nervous system's unconscious way of scanning for danger. Mine was misfiring constantly, interpreting neutral situations as threats. No wonder I couldn't relax—my body thought it was under siege.
Therapy helped, but so did learning to work with my body. Breathwork, grounding exercises, and even humming helped activate my vagus nerve and shift me toward calm. I started tracking my triggers, not just emotionally but physiologically. I learned that anxiety wasn't just in my head—it was in my nervous system, and I could retrain it.
"Living in a Body That Won't Power Down"
"Sometimes I feel kind of separate from myself, going through the motions, barely enough energy to do anything"
I used to love going hiking with my partner but since I was attacked and robbed in town, even though it was months ago, I don't seem to have the same interest in the hiking or spending time together. My chest feels heavy most of the time and trying to make a decision about the smallest things, seems so difficult. I've also noticed I am reluctant to meet up with my friends as I'm so down, the thought of having to do my hair and put on the makeup just seems to much effort, actually I can't remember the last time I went to the hairdressers.
Understanding the freeze response and the sensations in my body has helped me recognise that my body felt threatened, that my nervous system was doing what it was supposed to do and was trying to protect me. However, instead of helping me, my nervous system had become unhelpful. Working with my body with a specialist in body work has helped me recognise the signals and over time, with some somatic work, I have become more regulated and I am hiking again and spending time with my partner and friends.
You may wish to seek a somatic/body focused therapist or try Tai Chi, Qi Gong, Yoga which all help you get in touch with your body.. Also go to Create My Toolbox for some exercises in breathwork and mindfulness which can be helpful.
